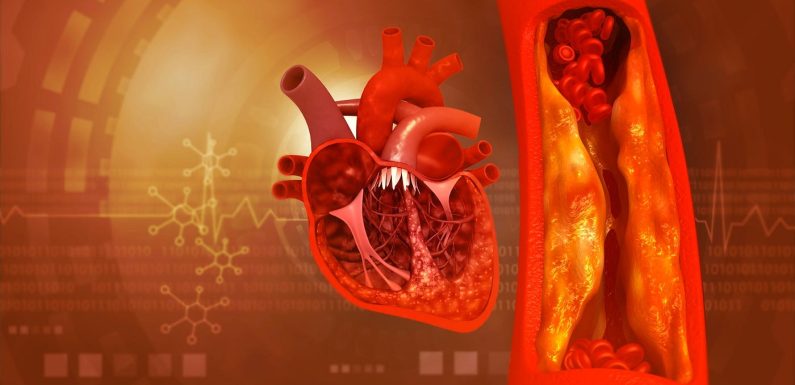
Plaque in arteries is atherosclerosis. It is a chronic disease that threatens cardiovascular health. Platelet activation is one of its reasons. Antiplatelet drugs are vital for treating and preventing atherosclerosis. Therefore, this article discusses antiplatelet drugs’ role in preventing atherosclerosis, its common types, benefits, and risks.
Understanding Atherosclerosis
Atherosclerosis is comprehensible before considering antiplatelet drugs. Plaque slowly builds up in artery walls in Atherosclerosis. So, calcium deposits, inflammatory cells, cholesterol, and fatty substances make up this plaque. Afterwards, plaque narrows arteries, reducing heart and brain oxygen and blood flow.
Platelets in Atherosclerosis
Platelets are vital to hemostasis, or blood clotting. So, platelets attach to blood vessel walls and activate. So, this activation causes a blood clot, sealing the injury.
Platelets may activate in atherosclerosis due to arterial endothelium damage. Therefore, this activation may help produce blood clots in the arteries, causing heart attacks, strokes, and other cardiovascular events.
How Antiplatelet Drugs Work
Antiplatelet drugs reduce platelet activation and aggregation. This reduces blood clots in atherosclerotic arteries, improving blood flow. In brief, Antiplatelet drugs have various types and different mechanisms:
P2Y12 inhibitors
Brilinta, Effient, and Plavix are P2Y12 inhibitors. They block the platelet-stimulating chemical signal ADP. So, Platelets’ P2Y12 receptor is blocked by these drugs, preventing clot formation.
3a/GP IIb Inhibitors
Tirofiban (Aggrastat), eptifibatide (Integrilin), and abciximab (ReoPro) target platelets’ GP IIb/IIIa receptor, which is needed for aggregation. GP IIb/IIIa inhibitors bind to this receptor to block the final platelet aggregation pathway.
Antiplatelet Drugs’ Atherosclerosis Prevention Benefits
Atherosclerosis management and prevention need antiplatelet drugs for several reasons.
Antiplatelet drugs reduce clot formation in damaged or limited arteries, preventing heart attacks and strokes. Therefore, they prevent platelet activation and aggregation.
Enhanced Circulation
Atherosclerosis-related blood flow improves by antiplatelet drugs, ensuring vital organs get adequate oxygen and nutrients.
Precaution Next
To reduce the risk of recurring heart attacks and strokes, antiplatelet medicines are routinely used.
Stent placement
Stent thrombosis and other complications following coronary artery stent or other interventional procedures are generally prevented using antiplatelet medicines.
To enhance cardiovascular health, antiplatelet medicines are commonly taken with lifestyle modifications, such as diet and exercise.
Risks and Issues
In short, Antiplatelet drugs have risks and adverse effects, including:
Gushing blood
High bleeding risk is a major problem with antiplatelet therapy. Secondly, this may involve bruises or worse issues including brain hemorrhage or gastrointestinal bleeding.
Reactions Allergic reactions to antiplatelet medicines are rare but may occur in certain individuals.
Drug Resistance
Some people’s antiplatelet therapy may not perform as effectively, reducing blood clot prevention.
Med-Drug Interactions
Antiplatelet drugs may interact with other drugs, lowering their efficacy or increasing bleeding risk.
Intestinal Harm
Aspirin, an antiplatelet, may cause stomach discomfort or ulcers.
Acceptance
Some persons may acquire immune to antiplatelet medications, requiring a change in treatment.
Personalized Antiplatelet Therapy
Each patient’s medical history, risk factors, and underlying conditions should determine their medication and antiplatelet pill choices. Therefore, healthcare providers assess the benefits of preventing clots against the risks of bleeding from antiplatelet therapy.
Antiplatelet therapy duration depends on the patient and scenario. Some patients require antiplatelet therapy permanently, while others need temporarily.
Conclusion
In short, Antiplatelet drugs improve blood flow to vital organs and reduce the risk of clots in damaged or constricted arteries, making them crucial for controlling and preventing atherosclerosis. Aspirin, P2Y12 inhibitors, and GP IIb/IIIa inhibitors reduce platelet activation and aggregation.

